Volume 7, Issue 1 (Autumn 2021)
Health in Emergencies and Disasters Quarterly 2021, 7(1): 5-14 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Peyravi M, Kharazmi E, Kavosi Z, Ahmadi Marzaleh M, Ghorbani Z. Estimation of Increasing the Surge Capacity of Shaheed Rajaei Trauma Hospital in Shiraz City, Iran. Health in Emergencies and Disasters Quarterly 2021; 7 (1) :5-14
URL: http://hdq.uswr.ac.ir/article-1-385-en.html
URL: http://hdq.uswr.ac.ir/article-1-385-en.html
Mahmoudreza Peyravi1 

 , Erfan Kharazmi2
, Erfan Kharazmi2 

 , Zahra Kavosi3
, Zahra Kavosi3 

 , Milad Ahmadi Marzaleh4
, Milad Ahmadi Marzaleh4 

 , Zahra Ghorbani *
, Zahra Ghorbani * 

 5
5


 , Erfan Kharazmi2
, Erfan Kharazmi2 

 , Zahra Kavosi3
, Zahra Kavosi3 

 , Milad Ahmadi Marzaleh4
, Milad Ahmadi Marzaleh4 

 , Zahra Ghorbani *
, Zahra Ghorbani * 

 5
5
1- Department of Health in Disasters and Emergencies, School of Management and Medical Informatics, Shiraz University of Medical Sciences, Shiraz, Iran.
2- Department of Health Management, School of Management and Medical Information Sciences, Shiraz University of Medical Sciences, Shiraz, Iran.
3- Health Human Resources Research Center, School of Management and Medical Informatics, Shiraz University of Medical Sciences, Shiraz, Iran.
4- Department of Health in Disasters and Emergencies, Health Human Resources Research Center, School of Management and Medical Informatics, Shiraz University of Medical Sciences, Shiraz, Iran.
5- Student Research Committee, Department of Health Care Management, Health Human Resources Research Center, School of Management and Medical Informatics, Shiraz University of Medical Sciences, Shiraz, Iran. ,z.ghorbani2014@gmail.com
2- Department of Health Management, School of Management and Medical Information Sciences, Shiraz University of Medical Sciences, Shiraz, Iran.
3- Health Human Resources Research Center, School of Management and Medical Informatics, Shiraz University of Medical Sciences, Shiraz, Iran.
4- Department of Health in Disasters and Emergencies, Health Human Resources Research Center, School of Management and Medical Informatics, Shiraz University of Medical Sciences, Shiraz, Iran.
5- Student Research Committee, Department of Health Care Management, Health Human Resources Research Center, School of Management and Medical Informatics, Shiraz University of Medical Sciences, Shiraz, Iran. ,
Full-Text [PDF 646 kb]
(694 Downloads)
| Abstract (HTML) (2042 Views)
Full-Text: (718 Views)
1. Introduction
Nowadays, accidents and disasters account for a large part of government resources and plans. Media provide information on various incidents around the world every day [1]. Usually, it is difficult to predict and manage incidents with mass casualties [2], and increasing population density has caused more people to be affected by large and small incidents [3]. The health area has a special status among all organizations involved in disaster management since the first and most important concern of people is health, and the preparedness to admit patients and increase the surge capacity in incidents and disasters are the main components of incident management [4]. Increasing hospital surge capacity during surging demand for a mass causality incident and accident is at the core of the hospital clinical responses [5]. During unexpected incidents and accidents, health and medical organizations should provide services beyond their regular capacity [6].
The Agency for Healthcare Research and Quality (AHRQ) has defined the surge capacity increase as the healthcare system’s capability to rapidly deploy services to respond to a sudden rise in demand for medical and health care during disasters [7]. Increasing surge capacity of the hospitals has been dramatically considered by planners [8]. As hospital surge capacity is a costly process, planners are responsible for achieving the optimum balance between the cost and demand in a disaster [9]. In a crisis situation, it is difficult for a health center to provide appropriate resources for all victims. However, as some hospitals are forced to provide both types of daily medical services during disasters, providing a quantitative model to predict if the existing assets are appropriate for disasters is of high importance [10].
The surge capacity of Carolina Teaching Hospital in Sweden in response to a simulated incident was based on an actual incident. During the study period, 59 operations could be performed [11]. Torab et al. reported that general hospitals showed no surge capacity given the physical aspects [12]. The lack of a standard method for calculating surge capacity is not surprising since increasing surge capacity is a relatively new term among medical terms [13]. Shiraz is a large City and medical pole in the southern part of Iran and annually attracts many people from the Persian Gulf countries for medical treatment, other provinces of Iran, and the cities of Fars Province. Also, Fars has experienced numerous natural and technological disasters in recent years, such as the flood event in 2001, the bombing of Hosseiniyeh Shohada in 2009, and the bus accident in 2014. So, it is necessary to pay attention to increasing the surge capacity of Shiraz hospitals in accidents and disasters.
Objectives
Given the need to increase hospital surge capacity during accidents and its vital role in responding to disasters, the present study was conducted to estimate the surge capacity of Shahid Rajaee Trauma Hospital in Shiraz in response to an incident in 2017.
2. Materials and Methods
Study design
This research is a descriptive study carried out in 2017 in Shahid Rajaee Level-2 Trauma Hospital. The research tool is a descriptive translation checklist that has been evaluated using the Delphi method for the validity and reliability of the tool. The steps of the methods are as follows: 1. translating the checklist into Persian and English, 2. calculating the reliability and validity of the checklist through the Delphi expert round, 3. scenario design for trauma hospital, and 4. calculating the need to increase capacity in the field of human resources, equipment, and operating room.
This hospital is the only trauma hospital in Shiraz and the primary referral center for trauma in the south of Iran. It is equipped with 400 beds, 53 intensive care beds, and 10 operating rooms. Under normal conditions, the bed occupancy rate was 75% in the studied hospital. The present study was conducted on three units of emergency room, operating room, and intensive care unit. The reason for selecting these three units is their direct and effective relationship with saving the lives of injured patients in the first exposure after they arrived in the hospital [11, 14]. In this study, a scenario was developed based on the global standard triage, as presented in Table 1.
.jpg)
Study measurement
The Delphi technique was used to collect the study data. This technique uses purposeful sampling, in which people who have extensive information about a particular phenomenon are used. In the present study, the method was used to estimate the human resources, equipment, skills, and time needed to provide services in the face of an unexpected incident during two rounds for the three teams of emergency, the operating room, and the intensive care unit. The agreement level for the Delphi rounds was considered 80%, and all calculations were done within a time interval of 30 minutes to 3 hours. First, the researcher referred to the Nursing Office and Research Deputy of Shahid Rajaee Hospital in Shiraz and used the views of the Manager and Nursing Deputy and several physicians at Shahid Rajaee Hospital in Shiraz. Head nurses of Resuscitation and Screen Unit, Surgical Emergency Unit, Admissions 2 and 3, and Emergency Supervisors were selected for Delphi teams. Several nurses with more than 5 years of employment history in the Emergency Department, head nurses of all ICUs and several nurses with more than 5 years of employment history in ICUs along with head nurses and supervisors of the operating room, several anesthesiologists, attending physicians, and several operating room nurses with more than 5 years of employment history were selected using Delphi method.
In this scenario, only priority 1 and priority 2 patients with the highest need for medical care were included in the analysis. The zero time in this scenario was defined as the patient’s arrival time at the hospital. As only the patients with priorities 1 and 2 were included in the study according to the global standard triage, first, these patients were defined in this section. Then, questions were asked regarding the three parts of the staff, equipment, resources, and time.
For this purpose, the checklists were translated from the original language into Persian. After the review, the original translated version was translated from the Persian language into the target language by the translator, who was not present at the previous stage. After its second review, the checklist was re-translated from the original language into the Persian language. Their validity and reliability were also examined. Table 2 lists the number of questions in each section.
.jpg)
In the first phase of Delphi, the checklists were given to 30 experts in each section. After collecting the checklists, the information derived from the emergency checklists, ICU, and operating room in the first round was entered into SPSS18 software and analyzed. This article was extracted from a Master thesis entitled “investigating the surge capacity of Shahid Rajaee Trauma Hospital in Shiraz in response to an unexpected accident in 2016” under the ethical code 10428.
Accordingly, the percentage of agreement among the members of the Delphi team was determined for each question, and the general agreement (in percentage) for each team was determined. The condition for stopping the Delphi method in this study was more than 80% agreement [12]. Finally, the results of the Delphi survey and the hospital basic information were used as the input of the present study.
Calculation of surge capacity
The basis of all calculations in this study was a crisis status [14]. By reviewing similar studies, the formulas needed to calculate the surge capacity of Shahid Rajaee Hospital in Shiraz were developed. Because no acceptable standard and model has been designed so far for determining the general surge capacity of the hospital, we developed the formulas needed for this hospital after studying similar samples.
Emergency Room
The number of physicians needed to deliver services for patients with the priority 1:
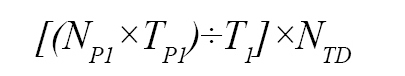
NP1= the total number of priority 1 patients.
TP1= the total time passed for each patient.
T1= the time needed to save the life of priority 1 patients.
NTD= the total number of physicians in each team.
The number of nurses needed to deliver services for patients with the priority 1:

NTN= the total number of nurses in each team.
The number of physicians needed to deliver services for patients with the priority 2:

NP2= the total number of priority 2 patients.
TP2= the total time passed for each patient.
T2= the time needed to save the life of priority 1 patients
The number of nurses needed to deliver services for patients with the priority 2:

NTN= the total number of nurses in each team
The number of nurses needed to deliver services for patients with the priority 1:
The total number of physicians needed to treat patients P1 and P2:
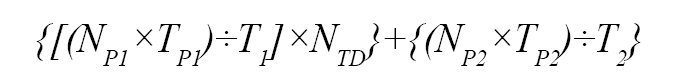
The total number of nurses needed to deliver services for patients P1:

NTN= the total number of nurses in each team.
Surge capacity of the emergency room
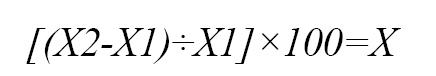
X= the percentage of surge capacity of the emergency department.
X1= the maximum number of patients admitted to the emergency.
X2= the total number of priority 1 and priority 2 patients calculated in the scenario who can be admitted.
The total number of physicians needed to deliver services to ICU patients in response to an unexpected incident:
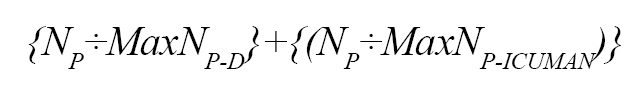
NP= the total number of patients admitted based on the scenario.
MaxNP-D = the maximum number of patients per ICU workers.
The total number of nurses needed to deliver services for ICU patients in response to an unexpected incident:

MaxNP-N=the maximum number of patients per nurse.
MaxNonICU-ICU= the maximum number of non-ICU nurses per ICU nurse.
Surge capacity of intensive care units
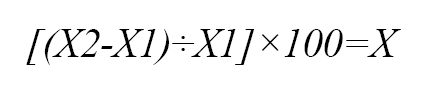
X=the percentage of surge capacity of ICU.
X1=the maximum number of patients in ICU.
X2=the total number of patients who can be admitted when faced with a crisis.
Surge capacity of the operating room
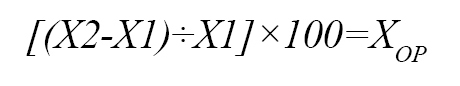
XOP= the percentage of surge capacity of the operating room.
X1= the maximum number of operations performed in the hospital within 12 hours.
X2= the total number of operations that can be performed within 12 hours.
Total surge capacity:
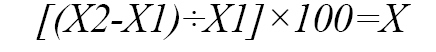
X = the percentage of total surge capacity.
The maximum number of interventions that can be done based on the space within the first 12 hours is:
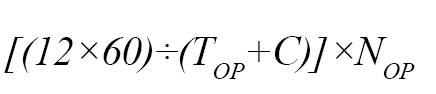
TOP= the duration of each intervention to save the life.
C= the time needed to prepare the operating room for the next operation.
NOP= the number of operating rooms.
Ethical considerations
The present study was approved by the Ethics Committee in biomedical research. In this regard, the participants were allowed to leave the study if they would like to. They were assured about the confidentiality of their information, with their names never being disclosed anywhere.
3. Results
Table 3 presents the demographic characteristics of the study participants.
.jpg)
The age range of the participants in the Delphi Emergency Team was 26-45 years, and their Mean±SD age was 32±4.25 years. The employment history of people in the Delphi Emergency Team was 5-15 years, with a mean of 8.82±2.02 years.
The Delphi checklist was developed with the characteristics described in Table 2. To determine the face validity, we sent a checklist to 4 experts in different fields. By specifying the defects and correcting them, and final confirmation of the checklist by experts, the face validity of the checklist was determined. To determine the reliability, 30 checklists (10 emergency checklists, 10 ICU checklists, and 10 operating room checklists) were distributed as a pilot among 30 members of Delphi teams. Checklists were collected at intervals of 1 week, and the data in the checklist were entered into SPSS v. 18 software. Then, a statistics consultant determined the Cronbach α values of 0.71, 0.677, and 0.74 for the emergency checklist, ICU checklist, and operating room checklist, respectively. It was found that all three checklists had acceptable reliability.
For each Delphi team, an agreement level of 80% was estimated. For this purpose, considering the probability of dropout in participants, 30 respondents (a total of 90 respondents) were included. Out of 30 participants in the Delphi team, 25 subjects in the Emergency Department, 29 in the ICU Delphi team, and 24 in the Operation Room Delphi team answered the questions. The agreement level in the first round was 60% for the emergency checklist, 56% for the ICU checklist, and 65.87% for the operating room checklist, so the Delphi round continued. In the second phase, Delphi was given to the same specialists one month later. Data of the second round were entered into the SPSS18 software and analyzed. Accordingly, the agreement level in the second round was 82.43% in the Emergency Department checklist, 80.6% in the ICU checklist, and 88.28% in the Operating Room checklist. As the condition for stopping the Delphi method in the current study was the general agreement level of more than 80%, with a general agreement of 82.43% among the members of the Emergency Department Delphi team, 80.6% among the members of the ICU Delphi team, and 88.28% among Operating Room Delphi team members in the second round, a consensus among members of the Delphi team was obtained. Finally, the results of Delphi and hospital basic information were used as input of this study.
Surge capacity in different units
Emergency department
The number of physicians needed to deliver services for patients with the priority 1:
- The total number of physicians needed in the first 60 minutes was

- The total number of physicians needed in the first 120 minutes was

- The mean number of physicians needed was
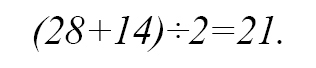
- The mean number of physicians needed for priority 1 patients in the mean time of 90 minutes was
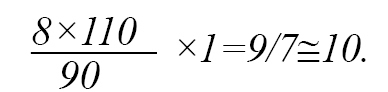
-The total number of physicians needed in the first 120 minutes was
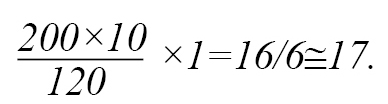
There are 40 stretchers available in the Emergency Department of Shahid Rajaee Hospital in Shiraz City that can be increased to 50 stretchers in emergencies. The patient’s stay on each stretcher is 4 hours. Therefore, in 2 hours, according to the number of stretchers, only 50 patients can be admitted. Also, to save the lives of 50 priority 2 patients in 120 minutes, 4 physicians are needed.

- The total number of physicians needed in 720 minutes was

The mean number of physicians needed was
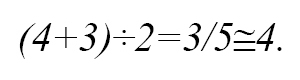
Four physicians can visit 120 patients in a mean time of 300 minutes (an average of 300 minutes was defined to save the life of P2 patients).
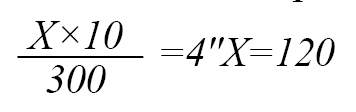
The total number of physicians needed to treat patients P1 and P2 was

The total number of nurses needed to provide service for patients P1:
- The total number of nurses needed in the first 60 minutes was

- The total number of nurses needed in the first 120 minutes was

The mean number of nurses needed was

As shown in Table 4, there are 4 recovery beds for priority 1 patients, and the number of beds can be increased up to 8 beds along with vital equipment in the first 2 hours in the hospital, so only 8 patients with priority 1 can be admitted.
.jpg)
The total number of nurses needed to provide service for P2 patients was

There are 40 stretchers available in the Emergency Department of Shahid Rajaee Hospital in Shiraz, and it can be increased to 50 stretchers in emergencies, and the patient’s stay in each stretch is 4 hours. Therefore, in 2 hours, according to the number of stretchers, only 50 patients can be admitted, and to save the lives of 50 priority 2 patients in 120 minutes, 17 nurses are needed.
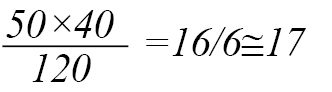
In Delphi, it was determined that the time needed to save the lives of priority 2 critically-ill patients is more than that required to save the lives of critically-injured patients. This time was obtained a minimum of 20 minutes for critically-injured patients and 40 minutes for critically ill patients.
-The total number of nurses needed in 720 minutes was

The mean number of nurses needed was

Thirteen nurses in the mean time of 300 minutes and mean service delivery time of 30 minutes can provide care for 130 patients.

The total number of nurses needed to provide service for P1 and P2 patients was
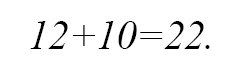
The calculations related to the maximum number of P2 patients, who can be admitted, are shown in Table 5.
.jpg)
Increasing the number of beds and equipment in the emergency department
The increase in the surge capacity depends on the ability to increase or maintain the resources. Crisis planners should recognize critical equipment and resources and consider them in crisis planning.
Table 6 presents the number of available equipment that can be increased separately for each unit in the emergency.
.jpg)
Increasing the surge capacity of emergencies was
Intensive Care Unit (ICU)
The number of ICU beds is one of the physical indicators of hospital capacity to care for injured casualties, although there is no international agreement [12]. The hospital has 53 beds in 6 specialized care units.
The total number of physicians needed to serve ICU patients in response to an unexpected incident was
.jpg)
Total number of nurses needed to deliver services for ICU patients in response to an unexpected incident
Table 7 presents information on the number of patients admitted to the intensive care unit.
.jpg)
Increasing capacity of ICU was:
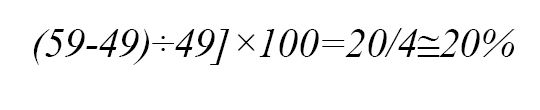
Considering the possibility of increasing the number of beds and patients in ICU, the results of this study showed that nurses with experience of working in ICU in the first degree and anesthesia and emergency nurses in the second degree of ICU are qualified to work in ICU under the supervision of ICU nurses. The ratio of ICU nurses to non-ICU nurses was 1 to 7. In this study, it was estimated that a non-ICU nurse needs one month of training to acquire basic skills for working in the unit in an unexpected incident, and the minimum nursing skills these nurses should acquire include assessment of the patient’s basic parameters, patient’s Glasgow Coma Scale (GCS), patient’s oxygen saturation (O2SAT), patient’s respiratory rate (RR), and completion of documents.
Increasing capacity of operating room
The best international models for incident events suggest that the number of operating rooms is one of the indicators showing the capacity to provide care in emergency and non-emergency situations [12]. The studied hospital has 10 operating rooms.

In this study, the maximum number of life-saving interventions in 12 hours was 47 operations, and increasing surge capacity for the operating room was obtained at 17.5.
Increasing the total surge capacity was
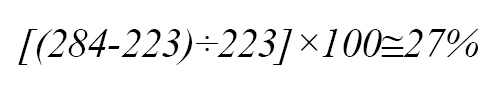
The maximum number of interventions that can be done within the first 12 hours based on the space is
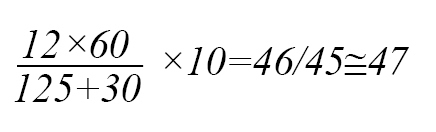
4. Discussion
Davis et al. found that about one-third of all patients admitted to the hospital within 24 hours could be discharged if faced with an incident. They also found that most patients could be discharged within 24 hours, and extra beds could be available [15]. In other studies, it has been reported that 20% of hospitalized patients can be discharged in a short period during the incidents [14]. On the other hand, in the London bombing in 2005, hospitals were criticized for discharging the patients to release the beds [16]. However, in the tsunami disaster in Southeast Asia in 2004, in six hospitals in Thailand with 1500 beds, more than 3000 patients were admitted in three days [17]. Compared with the present study, this study has a higher capacity to cope with disasters and crises.
Hirshberg et al., in a simulation study, showed that using the immediate resources available can estimated an unpredicted incident and a comprehensive program to cope with incidents increases the surge capacity by 7.1 times after deploying assets of the trauma hospital and on-call staff [18]. Higgins et al. reported an increase in the surge capacity of up to 27% of approved beds [19]. Thus, the surge capacity at 12 hours in Bayram et al.’s study was obtained higher than that of the present study.
Based on their experience in a trauma center, Eiseman et al. found that half of the trauma patients needed surgery in the first 12 hours [20, 21]. In the present study, the maximum number of life-saving interventions in 12 hours was obtained 47 operations. A review of the statistics in Shahid Rajaee Hospital Statistics Department showed that the maximum number of interventions in a working shift was 40 operations.
Many attempts have been made to calculate the surge capacity increase, but most studies have focused on only one component of the hospital and usually the emergency room, but the capability to increase the capacity depends on all the components of the hospital and, most importantly, on the three units of the Emergency Department, the Intensive Care Unit and the Operating Room. Robert Kanter et al. reported that New York City hospitals did not have an acceptable capacity to deliver services to children in unexpected incidents, and this capacity needs to be improved [22]. In the present study, the capacity to deliver services was estimated at a desirable level based on the defined scenario. In this study, we assumed that the staff was not a limiting factor and that the staff had adequate skills, but this assumption may be so optimistic and that a lot of staff might not have sufficient skills.
One of the limitations of this study was the inaccessibility to all intended experts and specialists. Therefore, we could not easily interact with them.
Study recommendations
1. Reopening of closed and non-clinical areas for the admission of emergency patients
2. Use of corridors for patient s’ admission
3- Altering the private rooms for the public rooms during the incident to increase the patients’ admission
4- The stretchers should be checked regularly to use the existing resources optimally in emergency conditions.
5. Conclusion
Increasing the surge capacity will be limited mainly due to the lack of immediate access to the beds, equipment, and human resources. Therefore, the studied hospital should look for solutions, including the surge capacity guidelines and more coordination between the hospital and prehospital emergency to increase its capacity and cope with unexpected incidents and accidents.
Ethical Considerations
Compliance with ethical guidelines
There were no ethical considerations to be considered in this research.
Funding
This project was supported by the Shiraz University of Medical Sciences.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest.
References
Nowadays, accidents and disasters account for a large part of government resources and plans. Media provide information on various incidents around the world every day [1]. Usually, it is difficult to predict and manage incidents with mass casualties [2], and increasing population density has caused more people to be affected by large and small incidents [3]. The health area has a special status among all organizations involved in disaster management since the first and most important concern of people is health, and the preparedness to admit patients and increase the surge capacity in incidents and disasters are the main components of incident management [4]. Increasing hospital surge capacity during surging demand for a mass causality incident and accident is at the core of the hospital clinical responses [5]. During unexpected incidents and accidents, health and medical organizations should provide services beyond their regular capacity [6].
The Agency for Healthcare Research and Quality (AHRQ) has defined the surge capacity increase as the healthcare system’s capability to rapidly deploy services to respond to a sudden rise in demand for medical and health care during disasters [7]. Increasing surge capacity of the hospitals has been dramatically considered by planners [8]. As hospital surge capacity is a costly process, planners are responsible for achieving the optimum balance between the cost and demand in a disaster [9]. In a crisis situation, it is difficult for a health center to provide appropriate resources for all victims. However, as some hospitals are forced to provide both types of daily medical services during disasters, providing a quantitative model to predict if the existing assets are appropriate for disasters is of high importance [10].
The surge capacity of Carolina Teaching Hospital in Sweden in response to a simulated incident was based on an actual incident. During the study period, 59 operations could be performed [11]. Torab et al. reported that general hospitals showed no surge capacity given the physical aspects [12]. The lack of a standard method for calculating surge capacity is not surprising since increasing surge capacity is a relatively new term among medical terms [13]. Shiraz is a large City and medical pole in the southern part of Iran and annually attracts many people from the Persian Gulf countries for medical treatment, other provinces of Iran, and the cities of Fars Province. Also, Fars has experienced numerous natural and technological disasters in recent years, such as the flood event in 2001, the bombing of Hosseiniyeh Shohada in 2009, and the bus accident in 2014. So, it is necessary to pay attention to increasing the surge capacity of Shiraz hospitals in accidents and disasters.
Objectives
Given the need to increase hospital surge capacity during accidents and its vital role in responding to disasters, the present study was conducted to estimate the surge capacity of Shahid Rajaee Trauma Hospital in Shiraz in response to an incident in 2017.
2. Materials and Methods
Study design
This research is a descriptive study carried out in 2017 in Shahid Rajaee Level-2 Trauma Hospital. The research tool is a descriptive translation checklist that has been evaluated using the Delphi method for the validity and reliability of the tool. The steps of the methods are as follows: 1. translating the checklist into Persian and English, 2. calculating the reliability and validity of the checklist through the Delphi expert round, 3. scenario design for trauma hospital, and 4. calculating the need to increase capacity in the field of human resources, equipment, and operating room.
This hospital is the only trauma hospital in Shiraz and the primary referral center for trauma in the south of Iran. It is equipped with 400 beds, 53 intensive care beds, and 10 operating rooms. Under normal conditions, the bed occupancy rate was 75% in the studied hospital. The present study was conducted on three units of emergency room, operating room, and intensive care unit. The reason for selecting these three units is their direct and effective relationship with saving the lives of injured patients in the first exposure after they arrived in the hospital [11, 14]. In this study, a scenario was developed based on the global standard triage, as presented in Table 1.
.jpg)
Study measurement
The Delphi technique was used to collect the study data. This technique uses purposeful sampling, in which people who have extensive information about a particular phenomenon are used. In the present study, the method was used to estimate the human resources, equipment, skills, and time needed to provide services in the face of an unexpected incident during two rounds for the three teams of emergency, the operating room, and the intensive care unit. The agreement level for the Delphi rounds was considered 80%, and all calculations were done within a time interval of 30 minutes to 3 hours. First, the researcher referred to the Nursing Office and Research Deputy of Shahid Rajaee Hospital in Shiraz and used the views of the Manager and Nursing Deputy and several physicians at Shahid Rajaee Hospital in Shiraz. Head nurses of Resuscitation and Screen Unit, Surgical Emergency Unit, Admissions 2 and 3, and Emergency Supervisors were selected for Delphi teams. Several nurses with more than 5 years of employment history in the Emergency Department, head nurses of all ICUs and several nurses with more than 5 years of employment history in ICUs along with head nurses and supervisors of the operating room, several anesthesiologists, attending physicians, and several operating room nurses with more than 5 years of employment history were selected using Delphi method.
In this scenario, only priority 1 and priority 2 patients with the highest need for medical care were included in the analysis. The zero time in this scenario was defined as the patient’s arrival time at the hospital. As only the patients with priorities 1 and 2 were included in the study according to the global standard triage, first, these patients were defined in this section. Then, questions were asked regarding the three parts of the staff, equipment, resources, and time.
For this purpose, the checklists were translated from the original language into Persian. After the review, the original translated version was translated from the Persian language into the target language by the translator, who was not present at the previous stage. After its second review, the checklist was re-translated from the original language into the Persian language. Their validity and reliability were also examined. Table 2 lists the number of questions in each section.
.jpg)
In the first phase of Delphi, the checklists were given to 30 experts in each section. After collecting the checklists, the information derived from the emergency checklists, ICU, and operating room in the first round was entered into SPSS18 software and analyzed. This article was extracted from a Master thesis entitled “investigating the surge capacity of Shahid Rajaee Trauma Hospital in Shiraz in response to an unexpected accident in 2016” under the ethical code 10428.
Accordingly, the percentage of agreement among the members of the Delphi team was determined for each question, and the general agreement (in percentage) for each team was determined. The condition for stopping the Delphi method in this study was more than 80% agreement [12]. Finally, the results of the Delphi survey and the hospital basic information were used as the input of the present study.
Calculation of surge capacity
The basis of all calculations in this study was a crisis status [14]. By reviewing similar studies, the formulas needed to calculate the surge capacity of Shahid Rajaee Hospital in Shiraz were developed. Because no acceptable standard and model has been designed so far for determining the general surge capacity of the hospital, we developed the formulas needed for this hospital after studying similar samples.
Emergency Room
The number of physicians needed to deliver services for patients with the priority 1:
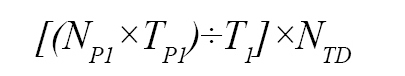
NP1= the total number of priority 1 patients.
TP1= the total time passed for each patient.
T1= the time needed to save the life of priority 1 patients.
NTD= the total number of physicians in each team.
The number of nurses needed to deliver services for patients with the priority 1:

NTN= the total number of nurses in each team.
The number of physicians needed to deliver services for patients with the priority 2:

NP2= the total number of priority 2 patients.
TP2= the total time passed for each patient.
T2= the time needed to save the life of priority 1 patients
The number of nurses needed to deliver services for patients with the priority 2:

NTN= the total number of nurses in each team
The number of nurses needed to deliver services for patients with the priority 1:
The total number of physicians needed to treat patients P1 and P2:
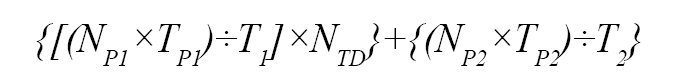
The total number of nurses needed to deliver services for patients P1:

NTN= the total number of nurses in each team.
Surge capacity of the emergency room
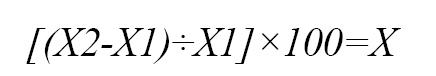
X= the percentage of surge capacity of the emergency department.
X1= the maximum number of patients admitted to the emergency.
X2= the total number of priority 1 and priority 2 patients calculated in the scenario who can be admitted.
The total number of physicians needed to deliver services to ICU patients in response to an unexpected incident:
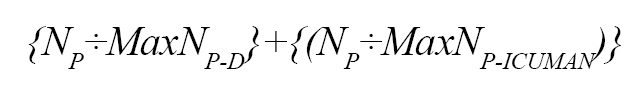
NP= the total number of patients admitted based on the scenario.
MaxNP-D = the maximum number of patients per ICU workers.
The total number of nurses needed to deliver services for ICU patients in response to an unexpected incident:

MaxNP-N=the maximum number of patients per nurse.
MaxNonICU-ICU= the maximum number of non-ICU nurses per ICU nurse.
Surge capacity of intensive care units
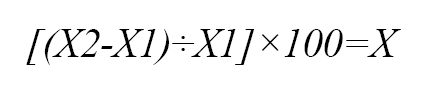
X=the percentage of surge capacity of ICU.
X1=the maximum number of patients in ICU.
X2=the total number of patients who can be admitted when faced with a crisis.
Surge capacity of the operating room
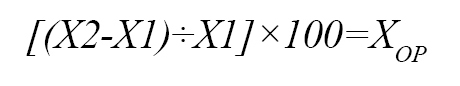
XOP= the percentage of surge capacity of the operating room.
X1= the maximum number of operations performed in the hospital within 12 hours.
X2= the total number of operations that can be performed within 12 hours.
Total surge capacity:
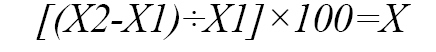
X = the percentage of total surge capacity.
The maximum number of interventions that can be done based on the space within the first 12 hours is:
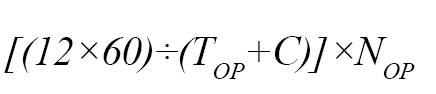
TOP= the duration of each intervention to save the life.
C= the time needed to prepare the operating room for the next operation.
NOP= the number of operating rooms.
Ethical considerations
The present study was approved by the Ethics Committee in biomedical research. In this regard, the participants were allowed to leave the study if they would like to. They were assured about the confidentiality of their information, with their names never being disclosed anywhere.
3. Results
Table 3 presents the demographic characteristics of the study participants.
.jpg)
The age range of the participants in the Delphi Emergency Team was 26-45 years, and their Mean±SD age was 32±4.25 years. The employment history of people in the Delphi Emergency Team was 5-15 years, with a mean of 8.82±2.02 years.
The Delphi checklist was developed with the characteristics described in Table 2. To determine the face validity, we sent a checklist to 4 experts in different fields. By specifying the defects and correcting them, and final confirmation of the checklist by experts, the face validity of the checklist was determined. To determine the reliability, 30 checklists (10 emergency checklists, 10 ICU checklists, and 10 operating room checklists) were distributed as a pilot among 30 members of Delphi teams. Checklists were collected at intervals of 1 week, and the data in the checklist were entered into SPSS v. 18 software. Then, a statistics consultant determined the Cronbach α values of 0.71, 0.677, and 0.74 for the emergency checklist, ICU checklist, and operating room checklist, respectively. It was found that all three checklists had acceptable reliability.
For each Delphi team, an agreement level of 80% was estimated. For this purpose, considering the probability of dropout in participants, 30 respondents (a total of 90 respondents) were included. Out of 30 participants in the Delphi team, 25 subjects in the Emergency Department, 29 in the ICU Delphi team, and 24 in the Operation Room Delphi team answered the questions. The agreement level in the first round was 60% for the emergency checklist, 56% for the ICU checklist, and 65.87% for the operating room checklist, so the Delphi round continued. In the second phase, Delphi was given to the same specialists one month later. Data of the second round were entered into the SPSS18 software and analyzed. Accordingly, the agreement level in the second round was 82.43% in the Emergency Department checklist, 80.6% in the ICU checklist, and 88.28% in the Operating Room checklist. As the condition for stopping the Delphi method in the current study was the general agreement level of more than 80%, with a general agreement of 82.43% among the members of the Emergency Department Delphi team, 80.6% among the members of the ICU Delphi team, and 88.28% among Operating Room Delphi team members in the second round, a consensus among members of the Delphi team was obtained. Finally, the results of Delphi and hospital basic information were used as input of this study.
Surge capacity in different units
Emergency department
The number of physicians needed to deliver services for patients with the priority 1:
- The total number of physicians needed in the first 60 minutes was

- The total number of physicians needed in the first 120 minutes was

- The mean number of physicians needed was
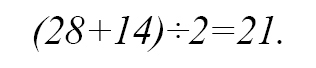
- The mean number of physicians needed for priority 1 patients in the mean time of 90 minutes was
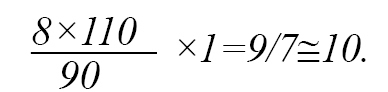
-The total number of physicians needed in the first 120 minutes was
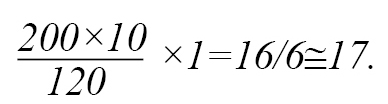
There are 40 stretchers available in the Emergency Department of Shahid Rajaee Hospital in Shiraz City that can be increased to 50 stretchers in emergencies. The patient’s stay on each stretcher is 4 hours. Therefore, in 2 hours, according to the number of stretchers, only 50 patients can be admitted. Also, to save the lives of 50 priority 2 patients in 120 minutes, 4 physicians are needed.

- The total number of physicians needed in 720 minutes was

The mean number of physicians needed was
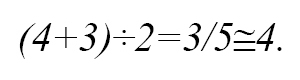
Four physicians can visit 120 patients in a mean time of 300 minutes (an average of 300 minutes was defined to save the life of P2 patients).
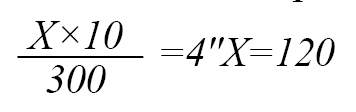
The total number of physicians needed to treat patients P1 and P2 was

The total number of nurses needed to provide service for patients P1:
- The total number of nurses needed in the first 60 minutes was

- The total number of nurses needed in the first 120 minutes was

The mean number of nurses needed was

As shown in Table 4, there are 4 recovery beds for priority 1 patients, and the number of beds can be increased up to 8 beds along with vital equipment in the first 2 hours in the hospital, so only 8 patients with priority 1 can be admitted.
.jpg)
The total number of nurses needed to provide service for P2 patients was

There are 40 stretchers available in the Emergency Department of Shahid Rajaee Hospital in Shiraz, and it can be increased to 50 stretchers in emergencies, and the patient’s stay in each stretch is 4 hours. Therefore, in 2 hours, according to the number of stretchers, only 50 patients can be admitted, and to save the lives of 50 priority 2 patients in 120 minutes, 17 nurses are needed.
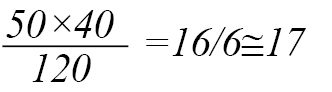
In Delphi, it was determined that the time needed to save the lives of priority 2 critically-ill patients is more than that required to save the lives of critically-injured patients. This time was obtained a minimum of 20 minutes for critically-injured patients and 40 minutes for critically ill patients.
-The total number of nurses needed in 720 minutes was

The mean number of nurses needed was

Thirteen nurses in the mean time of 300 minutes and mean service delivery time of 30 minutes can provide care for 130 patients.

The total number of nurses needed to provide service for P1 and P2 patients was
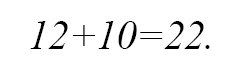
The calculations related to the maximum number of P2 patients, who can be admitted, are shown in Table 5.
.jpg)
Increasing the number of beds and equipment in the emergency department
The increase in the surge capacity depends on the ability to increase or maintain the resources. Crisis planners should recognize critical equipment and resources and consider them in crisis planning.
Table 6 presents the number of available equipment that can be increased separately for each unit in the emergency.
.jpg)
Increasing the surge capacity of emergencies was
Intensive Care Unit (ICU)
The number of ICU beds is one of the physical indicators of hospital capacity to care for injured casualties, although there is no international agreement [12]. The hospital has 53 beds in 6 specialized care units.
The total number of physicians needed to serve ICU patients in response to an unexpected incident was
.jpg)
Total number of nurses needed to deliver services for ICU patients in response to an unexpected incident
Table 7 presents information on the number of patients admitted to the intensive care unit.
.jpg)
Increasing capacity of ICU was:
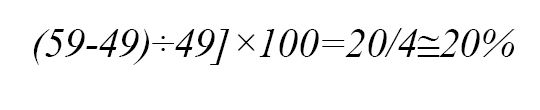
Considering the possibility of increasing the number of beds and patients in ICU, the results of this study showed that nurses with experience of working in ICU in the first degree and anesthesia and emergency nurses in the second degree of ICU are qualified to work in ICU under the supervision of ICU nurses. The ratio of ICU nurses to non-ICU nurses was 1 to 7. In this study, it was estimated that a non-ICU nurse needs one month of training to acquire basic skills for working in the unit in an unexpected incident, and the minimum nursing skills these nurses should acquire include assessment of the patient’s basic parameters, patient’s Glasgow Coma Scale (GCS), patient’s oxygen saturation (O2SAT), patient’s respiratory rate (RR), and completion of documents.
Increasing capacity of operating room
The best international models for incident events suggest that the number of operating rooms is one of the indicators showing the capacity to provide care in emergency and non-emergency situations [12]. The studied hospital has 10 operating rooms.

In this study, the maximum number of life-saving interventions in 12 hours was 47 operations, and increasing surge capacity for the operating room was obtained at 17.5.
Increasing the total surge capacity was
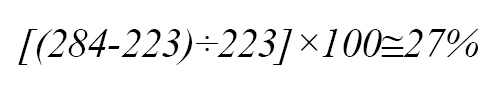
The maximum number of interventions that can be done within the first 12 hours based on the space is
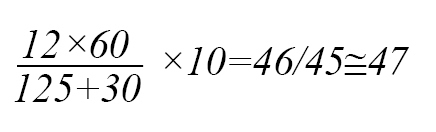
4. Discussion
Davis et al. found that about one-third of all patients admitted to the hospital within 24 hours could be discharged if faced with an incident. They also found that most patients could be discharged within 24 hours, and extra beds could be available [15]. In other studies, it has been reported that 20% of hospitalized patients can be discharged in a short period during the incidents [14]. On the other hand, in the London bombing in 2005, hospitals were criticized for discharging the patients to release the beds [16]. However, in the tsunami disaster in Southeast Asia in 2004, in six hospitals in Thailand with 1500 beds, more than 3000 patients were admitted in three days [17]. Compared with the present study, this study has a higher capacity to cope with disasters and crises.
Hirshberg et al., in a simulation study, showed that using the immediate resources available can estimated an unpredicted incident and a comprehensive program to cope with incidents increases the surge capacity by 7.1 times after deploying assets of the trauma hospital and on-call staff [18]. Higgins et al. reported an increase in the surge capacity of up to 27% of approved beds [19]. Thus, the surge capacity at 12 hours in Bayram et al.’s study was obtained higher than that of the present study.
Based on their experience in a trauma center, Eiseman et al. found that half of the trauma patients needed surgery in the first 12 hours [20, 21]. In the present study, the maximum number of life-saving interventions in 12 hours was obtained 47 operations. A review of the statistics in Shahid Rajaee Hospital Statistics Department showed that the maximum number of interventions in a working shift was 40 operations.
Many attempts have been made to calculate the surge capacity increase, but most studies have focused on only one component of the hospital and usually the emergency room, but the capability to increase the capacity depends on all the components of the hospital and, most importantly, on the three units of the Emergency Department, the Intensive Care Unit and the Operating Room. Robert Kanter et al. reported that New York City hospitals did not have an acceptable capacity to deliver services to children in unexpected incidents, and this capacity needs to be improved [22]. In the present study, the capacity to deliver services was estimated at a desirable level based on the defined scenario. In this study, we assumed that the staff was not a limiting factor and that the staff had adequate skills, but this assumption may be so optimistic and that a lot of staff might not have sufficient skills.
One of the limitations of this study was the inaccessibility to all intended experts and specialists. Therefore, we could not easily interact with them.
Study recommendations
1. Reopening of closed and non-clinical areas for the admission of emergency patients
2. Use of corridors for patient s’ admission
3- Altering the private rooms for the public rooms during the incident to increase the patients’ admission
4- The stretchers should be checked regularly to use the existing resources optimally in emergency conditions.
5. Conclusion
Increasing the surge capacity will be limited mainly due to the lack of immediate access to the beds, equipment, and human resources. Therefore, the studied hospital should look for solutions, including the surge capacity guidelines and more coordination between the hospital and prehospital emergency to increase its capacity and cope with unexpected incidents and accidents.
Ethical Considerations
Compliance with ethical guidelines
There were no ethical considerations to be considered in this research.
Funding
This project was supported by the Shiraz University of Medical Sciences.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest.
References
- Khankah HR. [Hospital preparedness for disasters: A national program (Persian)]. Tehran: University of Social Welfare and Rehabilitation Sciences; 2016. http://opac.nlai.ir/opac-prod/bibliographic/3110444
- Culley J, McKnight S, Rivish VO, Moneda MD. Mass casualty information decision support. Online Journal of Nursing Informatics. 2015; 15(3). https://www.researchgate.net/publication/288439163_Mass_casualty_information_decision_support
- Welzel TB, Koenig KL, Bey T, Visser E. Effect of hospital staff surge capacity on preparedness for a conventional mass casualty event. Western Journal of Emergency Medicine. 2016; 11(2):189-96. [PMID] [PMCID]
- Khankeh HR, Mohammadi R, Ahmadi F. Health care services at time of natural disasters: A qualitative study. Iran Journal of Nursing. 2017; 20(51):85-96. https://ijn.iums.ac.ir/browse.php?a_code=A-10-1-213&sid=1&slc_lang=en
- Bayram JD, Zuabi S, Subbarao I. Disaster metrics: Quantitative benchmarking of hospital surge capacity in trauma-related multiple casualty events. Disaster Medicine and Public Health Preparedness. 2018; 5(02):117-24. [DOI:10.1001/dmp.2010.19] [PMID]
- Khademipour G, Sheikh Bardsiri H, Yar Mohammadian MH, Nekuyi Moghadam M. Hospitals capability in response to disasters considering surge capacity approach. Health in Emergencies & Disasters Quarterly. 2018; 1(2):111-8. http://hdq.uswr.ac.ir/article-1-85-en.html
- Kaji A, Koenig KL, Bey T. Surge capacity for healthcare systems: A conceptual framework. Academic Emergency Medicine. 2016; 13(11):1157-9. [DOI:10.1197/j.aem.2006.06.032] [PMID]
- Hick JL, Barbera JA, Kelen GD. Refining surge capacity: Conventional, contingency, and crisis capacity. Disaster Medicine and Public Health Preparedness. 2019; 3(S1):S59-67. [DOI:10.1097/DMP.0b013e31819f1ae2] [PMID]
- Jeffrey W, Runge MD. Surge medical response capability: What is it? How do we get it? How do we know when we have it? Washington (DC): National Academies Press (US); 2018. [PMID]
- Barbisch DF, Koenig KL. Understanding surge capacity: Essential elements. Academic Emergency Medicine. 2016; 13(11):1098-102. [DOI:10.1197/j.aem.2006.06.041] [PMID]
- Montán KL, Riddez L, Lennquist S, Olsberg A, Lindberg H, Gryth D, et al. Assessment of hospital surge capacity using the MACSIM simulation system: A pilot study. European Journal of Trauma and Emergency Surgery. 2017; 43(4):525-39. [DOI: 10.1007/s00068-016-0686-1] [PMID]
- Traub M, Bradt DA, Joseph AP. The surge capacity for people in emergencies (SCOPE) study in Australasian hospitals. Medical Journal of Australia. 2017; 186(8):394-8. [DOI:10.5694/j.1326-5377.2007.tb00971.x] [PMID]
- Schull MJ. Hospital surge capacity: If you can’t always get what you want, can you get what you need? Annals of Emergency Medicine. 2016; 48(4):389-90. [DOI:10.1016/j.annemergmed.2006.06.003] [PMID] [PMCID]
- Abir M, Davis MM, Sankar P, Wong AC, Wang SC. Design of a model to predict surge capacity bottlenecks for burn mass casualties at a large academic medical center. Prehospital and Disaster Medicine. 2019; 28(1):23-32. [DOI:10.1017/S1049023X12001513] [PMID]
- Davis DP, Poste JC, Hicks T, Polk D, Rymer TE, Jacoby I. Hospital bed surge capacity in the event of a mass-casualty incident. Prehospital and Disaster Medicine. 2015; 20(3):169-76. [DOI:10.1017/S1049023X00002405] [PMID]
- Aylwin CJ, König TC, Brennan NW, Shirley PJ, Davies G, Walsh MS, et al. Reduction in critical mortality in urban mass casualty incidents: Analysis of triage, surge, and resource use after the London bombings on July 7, 2005. The Lancet. 2017; 368(9554):2219-25. [DOI:10.1016/S0140-6736(06)69896-6]
- Lennquist S, Hodgetts T. Evaluation of the response of the Swedish healthcare system to the tsunami disaster in South East Asia. European Journal of Trauma and Emergency Surgery. 2018; 34(5):465-85. [DOI:10.1007/s00068-008-8807-0] [PMID]
- Hirshberg A, Scott BG, Granchi T, Wall Jr MJ, Mattox KL, Stein M. How does casualty load affect trauma care in urban bombing incidents? A quantitative analysis. Journal of Trauma and Acute Care Surgery. 2017; 58(4):686-95. [DOI:10.1097/01.TA.0000159243.70507.86] [PMID]
- Higgins W, Wainright C, Lu N, Carrico R. Assessing hospital preparedness using an instrument based on the mass casualty disaster plan checklist: Results of a statewide survey. American Journal of Infection Control. 2014; 32(6):327-32. [DOI:10.1016/j.ajic.2004.03.006] [PMID] [PMCID]
- Lynn M, Gurr D, Memon A, Kaliff J. Management of conventional mass casualty incidents: Ten commandments for hospital planning. Journal of Burn Care & Research. 2016; 27(5):649-58. [DOI:10.1097/01.BCR.0000238119.29269.2B] [PMID]
- Eiseman B, Moore EE, Meldrum DR, Raeburn C. Feasibility of damage control surgery in the management of military combat casualties. Archives of Surgery. 2020; 135(11):1323-7. [DOI:10.1001/archsurg.135.11.1323] [PMID]
- Kanter RK, Moran JR. Hospital emergency surge capacity: An empiric New York statewide study. Annals of Emergency Medicine. 2017; 50(3):314-9. [DOI:10.1016/j.annemergmed.2006.10.019] [PMID]
Type of Study: Research |
Subject:
Special
Received: 2021/08/31 | Accepted: 2021/09/2 | Published: 2021/10/1
Received: 2021/08/31 | Accepted: 2021/09/2 | Published: 2021/10/1
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |





